Nigeria has granted provisional approval to Oxford University’s R21 malaria vaccine, its medicines regulator said, making it the second country to do so after Ghana last week.
This was announced by the Director-General of the National Agency for Food and Drug Administration And Control (NAFDAC), Mojisola Adeyeye, during a press briefing on Monday, April 17, 2023.
Ghana became the first country to approve a highly effective malaria vaccine developed at Oxford university in the UK.
The R21/Matrix-M vaccine, the first to exceed the World Health Organization’s target of 75% efficacy, has been cleared for use by Ghana’s Food and Drugs Authority in children aged 5-36 months, the group at highest risk of death from malaria.
Prof Adrian Hill, the director of the Jenner Institute, which is part of the Nuffield Department of medicine at Oxford University, said: “This marks a culmination of 30 years of malaria vaccine research at Oxford with the design and provision of a high efficacy vaccine that can be supplied at adequate scale to the countries who need it most.”
However, observers warned it was “no silver bullet” in the complex fight against the mosquito-borne disease.
An estimated 619,000 people died from malaria in 2021, the vast majority of them children in sub-Saharan Africa, according to the WHO.
In Ghana, where the disease is both endemic and perennial, an estimated 5.3m cases and 12,500 estimated deaths were recorded, the Guardian reported.
The WHO has yet to recommend the R21 vaccine for widespread use and until it does there is a question mark over the amount of international funding available for it. The vaccine’s phase 3 trial is ongoing, but earlier trials have shown efficacy levels of 77%, a level maintained after a single booster dose given a year later.
In contrast, the RTS,S vaccine, which the WHO recommended for use in a landmark move in 2021, has more modest efficacy levels.
The Serum Institute of India, the biotechnology giant that is manufacturing the R21 vaccine, said it has the potential to manufacture more than 200m doses annually.
Adar Poonawalla, the CEO of the Serum Institute, said the licensure of the vaccine by Ghanaian authorities was a significant milestone in the fight against malaria.
The mosquito-borne disease kills more than 600,000 people each year, most of them African babies and children.
Nigeria, the continent’s most populous nation, was the world’s worst-affected country with 27% of global cases and 32% of global deaths, according to a 2021 World Health Organization (WHO) report on malaria.
“A provisional approval of the R21 Malaria Vaccine was recommended and this shall be done in line with the WHO’s Malaria Vaccine Implementation Guideline,” said Nigeria’s National Agency for Food and Drug Administration and Control.
“While granting the approval, the Agency has also communicated the need for expansion of the clinical trial conducted to include a phase 4 clinical trial/Pharmacovigilance study to be carried out in Nigeria,” its director-general Mojisola Christianah Adeyeye said in a statement.
It was unclear when the vaccine may be rolled out in Nigeria or Ghana as other regulatory bodies, including the WHO, are still assessing its safety and effectiveness, Reuters reported.
Childhood vaccines in the poorest parts of Africa are typically co-funded by international organisations such as Gavi, the vaccine alliance, only after getting WHO approval.
Mid-stage data from the R21 trial involving more than 400 young children was published in September, showing vaccine efficacy of between 70-80% at 12 months following the fourth dose.
Data from an ongoing phase 3 clinical trial involving 4,800 children in Burkina Faso, Kenya, Mali and Tanzania is due to be published in the coming months.
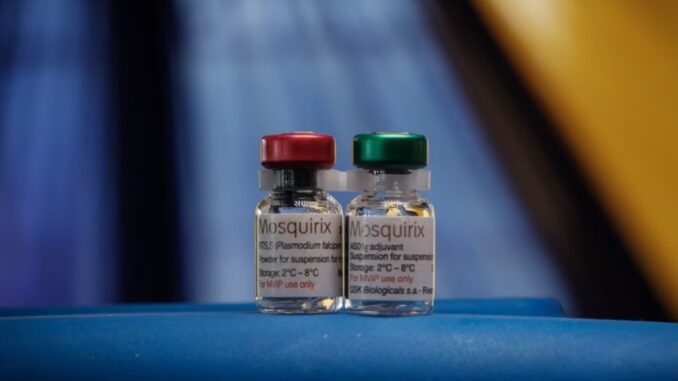
The first malaria vaccine, Mosquirix from British drugmaker GSK (GSK.L), was endorsed by the WHO last year after decades of work, but a lack of funding and commercial potential is thwarting GSK’s capacity to produce enough doses, demonstrating a need for another candidate.
Oxford has a deal with the Serum Institute of India to produce up to 200 million doses of R21 annually.




